

Professor Jacques Marescaux
President and founder of IRCAD
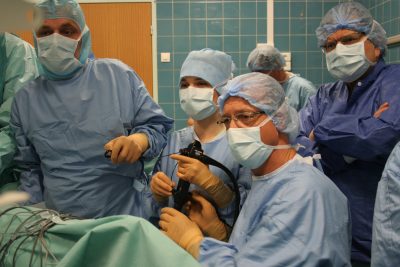
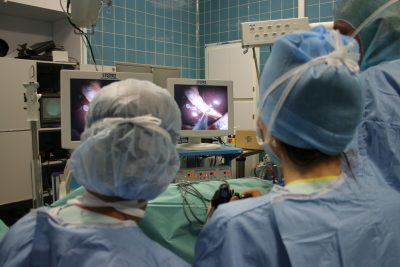
In April 2007, 16 years ago, IRCAD teams performed the first scarless surgery to remove a patient’s gallbladder through the vagina. This procedure, known worldwide as “Operation Anubis”, opened the way to a less invasive surgery, causing less pain and probably fewer complications, hence promoting outpatient procedures. Here is a glance back at this world first with Professor Jacques Marescaux, IRCAD President and Founder.
Professor Jacques Marescaux, how did you come up with this surgical approach known as Operation Anubis?
Operation Anubis is the first surgery performed without any external scar. We performed a cholecystectomy, which is the removal of the gallbladder without any incision, through the vagina. This concept originated from the achievements of Anthony Kalloo, an American gastroenterologist who, during a surgical conference, demonstrated the feasibility of the transgastric route to perform abdominal explorations or surgical interventions, and published these findings in Gastrointestinal Endoscopy in 2004. The concept was daring, especially from a gastroenterologist, since it involved damaging a healthy stomach to perform a surgical procedure. However, it was worth exploring to see if it could be beneficial to the patient (no scar, faster recovery, etc.). As a result, from 2005 onwards, IRCAD embarked on an intensive research program on transluminal endoscopic surgery through natural orifices. This program, called Anubis, was created to develop feasibility and survival studies, as well as new endoscopic technologies. Between 2004 and 2007, more than 500 NOTES (Natural Orifice Transluminal Endoscopic Surgery) procedures were performed in experimental models, including cholecystectomies, distal pancreatectomies, splenectomies, adrenalectomies, and bowel resections. This program was undertaken in collaboration with our industrial partners, as it was necessary to design suitable instruments to perform these operations. Of note, surgery requires the ability to reproduce the triangulation of the surgeon’s hand gestures. At the time, these instruments were lacking. The Anubis program has significantly contributed to accelerate innovation in surgical instrumentation. The first transvaginal cholecystectomy, performed on April 2, 2007, is a major milestone in the Anubis program, and more generally in the development of surgery through natural orifices.
What were the benefits of this scarless procedure for the patient?
First, the patient was delighted. She felt no pain, so she was ready to be discharged the following day, but we preferred to keep her for 48 hours for safety reasons. She was particularly happy that she would not have any scars or cosmetic after-effects. Cosmetically, but also psychologically speaking, it is essential for the patient to remain scarless after an intervention.
What was the impact of this first on surgical practice?
The Anubis program has driven technological advances in minimally invasive surgery with the introduction of new instruments. It has undeniably played a key role in accelerating the development of endoscopic surgery instruments. The access route through organs (in particular the vagina or the stomach) has not become widespread since the benefits were insufficient compared to laparoscopic surgery (abdominal keyhole surgery) regarding the complexity of the approach. However, the research undertaken has led us to develop systems which allow the scarring and healing of the keyholes in the organ.
It is now possible, even common, to remove small gastrointestinal tumors, i.e. in the rectum, colon, esophagus or stomach, through natural orifices. For patients, this changes everything —not only do these less invasive procedures reduce pain and accelerate recovery, but they also offer the possibility of preventing scars, which reflect the memory of the disease. Once healed, the patient can more easily move on. Finally, in morbidly obese patients, the approach developed over the last few years leading to an internal shrinkage of the stomach seems promising.
Are there any other minimally invasive approaches when natural orifice surgery is not possible?
Percutaneous surgery is the other rapidly growing specialty of minimally invasive surgery. This allows renal or hepatic tumors smaller than 1cm to be destroyed with a needle using cold (cryotherapy) or heat (radiofrequency). In the context of theDisrumpere project, IRCAD France and IRCAD Africa teams are developing technologies which facilitate the targeting and destruction of tumors. Our objective is to make this minimally invasive therapeutic modality accessible to non-expert operators to better meet the needs of patients worldwide, and to accelerate the development of treatments that will probably become the gold standard in the near future. However, to do so, we must be able to identify tumors at an early stage. The future of minimally invasive surgery, whether percutaneous or performed through natural orifices, is subsequently inextricably linked to diagnostic progress. IRCAD teams have developed several artificial intelligence systems which enable automatic diagnosis or screening of such small tumors. Likewise, several industrial companies have developed artificial intelligence systems which can detect tumors that are almost invisible to the human eye during a colonoscopy.
IRCAD research teams include doctors, engineers, and mathematicians who are enthusiastically committed to advancing these technologies, which will bring true benefits to patients and will probably generate savings for society as a whole in the long term.
Established in 1994 by Professor Jacques Marescaux, IRCAD is a specialized institution focused on advancing research and training in the field of minimally invasive surgery. Based in Strasbourg, IRCAD has gained global recognition for its exceptional training programs, which attract around 8,800 surgeons from across the world annually, both in-person and through the free online Websurg university, boasting over 470,000 registered members worldwide. Stay up-to-date with IRCAD’s latest developments on Twitter, Instagram, Facebook or LinkedIn.
For more information: https://www.ircad.fr/
Contacts for the press:
FINN Partners – sante@finnpartners.com

Please note that the IRCAD administrative board and staff are closely monitoring the evolving COVID-19 situation, in full compliance with all applicable laws and regulations in France. The health, safety, and well-being of our participants, experts and staff are our top priority!
Despite the current context, the IRCAD stands firmly by your side to help you acquire knowledge and skills. Come and join us !
We would like to draw your attention that the « Vaccine Pass » is now mandatory in France since end of January 2022 and replaces the former « Health Pass » to access places that are open to the public, such as cinemas, museums, cafés and restaurants, hotels as well as the IRCAD Institute which welcomes participants in the framework of its courses and seminars. Thus, a PCR test without vaccination is no longer sufficient to take part in our courses.
The vaccine pass includes a proof of the following (one of the 3 items is sufficient):
Further information about the new vaccine pass can be found at :
We very much hope to be able to count on your kind understanding of those rules which have been set by the French Government and which our Institute is required to apply